Dr. Digvijay Singh is a trusted glaucoma specialist in Delhi NCR, located in Gurgaon, treating patients suffering from all stages of glaucoma. As a glaucoma specialist near me, the doctor works to maximize a patient’s vision and preserve his/her quality of life using the latest advancements in diagnostic and treatment technologies. As a glaucoma eye specialist, he always tells the patients that glaucoma has to be managed and controlled from an early stage, and he provides them with a tailored approach to deal with all of their challenges.
Glaucoma Specialist in Gurgaon
Glaucoma is a serious eye condition that damages the optic nerve, often linked to high blood pressure, and is a leading cause of blindness in people over 60. Early detection is crucial. Dr. Digvijay Singh, a renowned glaucoma specialist in Gurgaon, India, has extensive experience treating hundreds of glaucoma cases. Known for his personalized care, advanced diagnostic methods, and dedication to early treatment, he is highly trusted by both patients and practitioners for providing effective glaucoma management.
Types of glaucoma
There are mainly 2 types of glaucoma
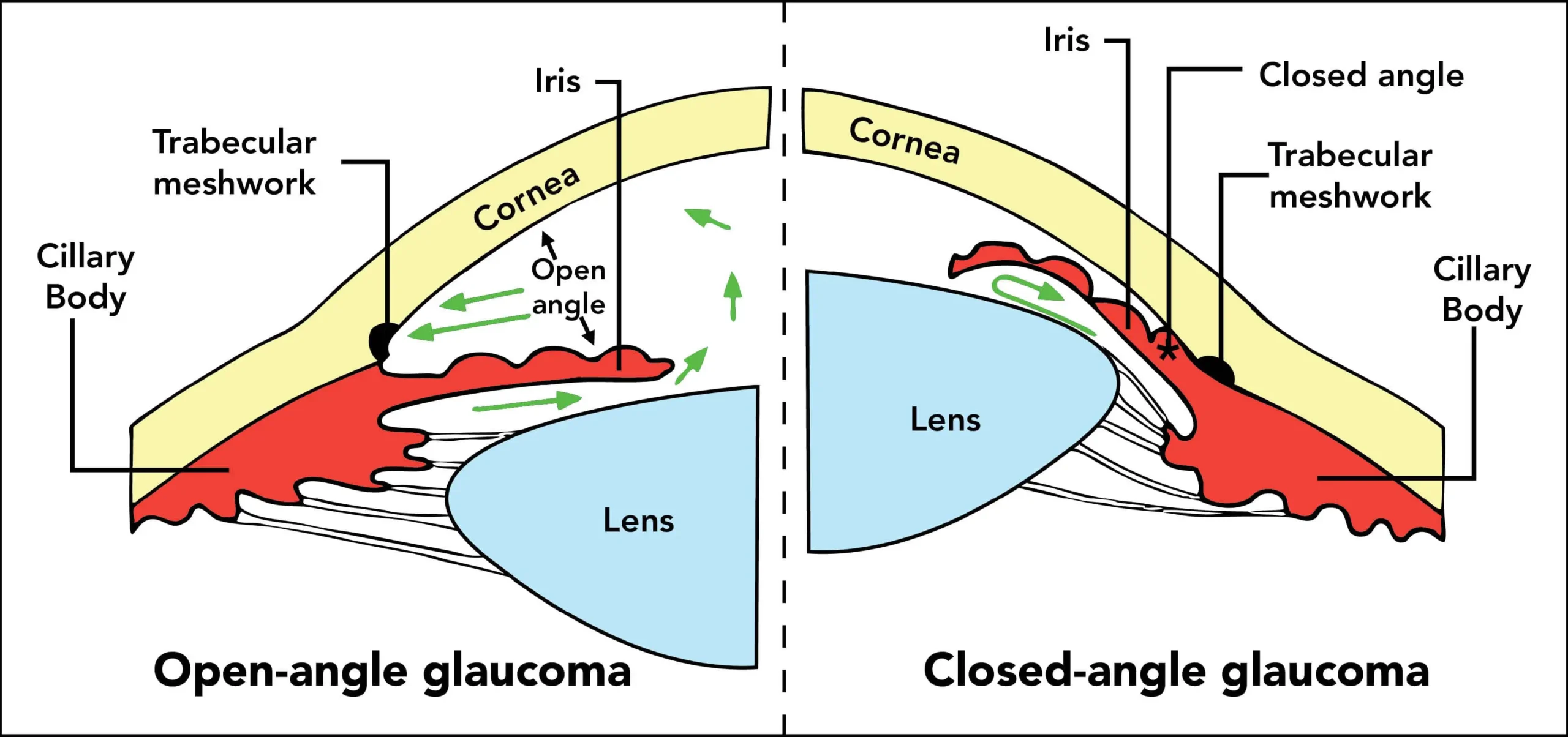
-
Open angle glaucoma
This is an asymptomatic form of glaucoma which often progresses to advanced stages before detection. However the progression of disease is slower than angle closure glaucoma and can be halted with proper medical and laser therapy. In advanced cases, surgery may be needed.
-
Narrow angle or closed angle glaucoma
People suffering from this form of glaucoma would experience pain, redness, and headache which would make you seek the help of an ophthalmologist. Some of these patients would see coloured halos around light bulbs in the evening time though it may also be asymptomatic. It can be treated with laser and may often require surgery.
Glaucoma Surgery Specialist Doctor
Dr. Digvijay Singh is a leading glaucoma surgery specialist in Gurgaon with nearly two decades of experience. Known for his patient-centered approach, he offers personalized treatment plans that address glaucoma effectively while ensuring long-term results. Staying updated with the latest surgical advancements, Dr. Singh provides precise, modern treatments, earning trust and high satisfaction from his patients.
Glaucoma can gradually damage vision without noticeable symptoms, especially in its early stages. In India, primary angle-closure glaucoma is as common as primary open-angle glaucoma and tends to be more symptomatic and vision-threatening.
Early diagnosis and treatment can minimize or prevent optic nerve damage and limit glaucoma-related vision loss. It's important to get your eyes examined regularly, and make sure your eye doctor measures your intraocular pressure.
Early Symptoms of Glaucoma
Primary open-angle glaucoma and Narrow angle glaucoma have completely different symptoms.
1. Primary open-angle glaucoma signs and symptoms include:
- Heaviness, eye pain.
- Gradual loss of peripheral vision, usually in both eyes
- Tunnel vision in the advanced stages
2. Narrow angle glaucoma signs and symptoms include:
- Eye pain
- Nausea and vomiting (accompanying the severe eye pain)
- Sudden onset of visual disturbance, often in low light
- Blurred vision
- Halos around lights
- Redness of the eye
Both open-angle and narrow angle glaucoma can be primary or secondary conditions. They're called primary when the cause is unknown and secondary when the condition can be traced to a known cause, such as eye injury, medications, certain eye conditions, inflammation, tumor, advanced cataract or diabetes. In secondary glaucoma, the signs and symptoms can include those of the primary condition as well as typical glaucoma symptoms. In a few cases, the glaucoma may be due to both open angle and narrow angle changes in which case it is termed a mixed glaucoma.

Test and diagnosis for glaucoma
Your doctor will review your medical history and conduct a comprehensive eye examination. Your doctor may perform several tests to diagnose glaucoma, including:
Visual acuity
Your doctor will test your ability to see from a distance. Measuring intraocular pressure by the Applanation Tonometer or the non contact Tonometer.
Tonometry is a simple, painless procedure that measures your internal eye pressure (intraocular pressure), after numbing your eyes with drops. It's usually the initial screening test for glaucoma.
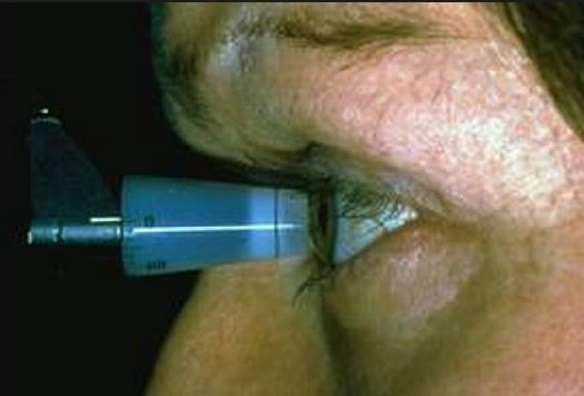
Test for optic nerve damage
To check for damage in your optic nerve, your eye doctor uses instruments to look directly through the pupil to the back of your eye(fundus). This can reveal slight changes that may indicate the beginnings of glaucoma.
Gonioscopy
The doctor will use a special instrument called a gonioscope to view inside your eye to distinguish between open-angle glaucoma and narrow angle glaucoma. The instrument will be gently placed upon the eye after putting some numbing drops for this test.
Visual field test using the Field analyzer
To check whether your visual field has been affected by glaucoma, your doctor uses a special test to evaluate your peripheral vision.
Measuring cornea thickness (pachymetry)
Your eyes are numbed for this test, which determines the thickness of each cornea, an important factor in diagnosing glaucoma. If you have thick corneas, your eye-pressure reading may read higher than normal even though you may not have glaucoma. Similarly, people with thin corneas can have normal pressure readings and still have glaucoma.
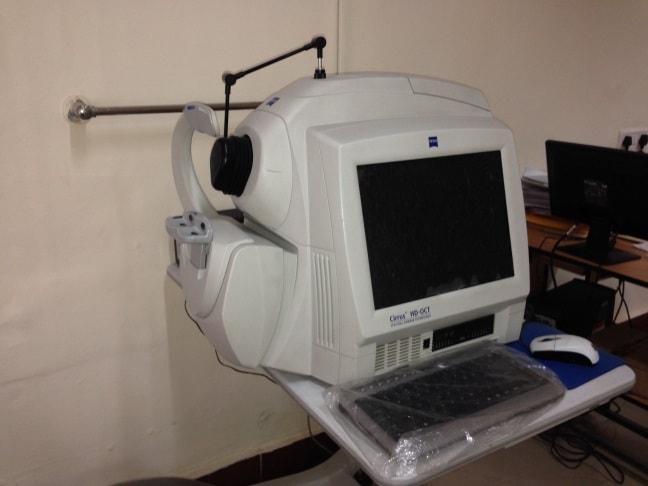
Special Imaging
Special imaging tests to evaluate the optic nerve for damage may be done by your eye doctor. These include non-invasive tests like the optical coherence tomography (OCT) and Heidelberg Retinal Tomography (HRT).
Treatments and drugs for glaucoma
The goal of glaucoma treatment is to lower pressure in your eye (intraocular pressure). To treat your condition, doctors may lower your eye pressure, improve drainage of fluid in your eye or lower the amount of fluid produced in your eye.
1. Eye-drops
Glaucoma treatment often starts with medicated eye-drops. Be sure to use the drops exactly as prescribed, otherwise, your optic nerve damage could get even worse. If your doctor prescribes more than one type of eye-drop, make sure to ask how long to wait between applications and to take the drops for as long as your doctor has prescribed them.
2. Oral medications
If eye-drops alone don't bring your eye pressure down to the desired level, your doctor may also prescribe oral medications, to reduce your eye pressure. These medications may cause side effects including nausea, vomiting, gastric upset, frequent urination, a tingling sensation in the fingers and toes, depression, stomach upset, and kidney stones.
3. Laser
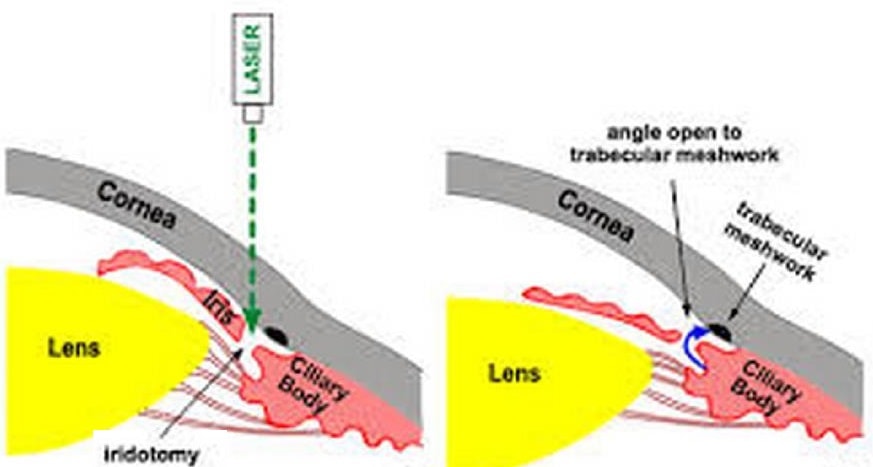
For open-angle glaucoma, laser trabeculoplasty uses a numbing drop and a laser to open clogged drainage canals and improve fluid outflow. For angle-closure glaucoma, laser peripheral iridotomy widens the angle to enhance drainage. Eye pressure is monitored for weeks, and long-term medications may be needed as pressure can rise over time.
4. Surgery
You may need surgery to treat glaucoma if you can't tolerate medications or if they're ineffective. Sometimes a single surgical procedure may not effectively lower your eye pressure. You may need to continue using eye-drops, or you may need another procedure.
Surgeries that may be performed to treat glaucoma include:
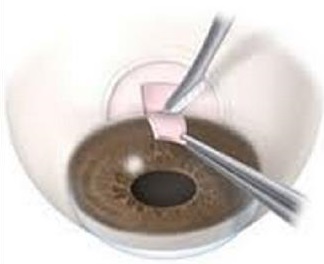
- Filtering surgery: If eye-drops and laser surgery don’t control eye pressure, a trabeculectomy may be needed. Performed outpatient under local anesthesia, the surgeon creates a small drainage opening in the eye, allowing fluid to exit and lowering pressure. Surgery is usually done one eye at a time. Follow-up visits are needed, with antibiotic and anti-inflammatory drops to prevent infection and scarring. Another option, trabeculotomy, removes a small section of the trabecular meshwork via a tiny corneal incision to improve fluid drainage and reduce eye pressure.
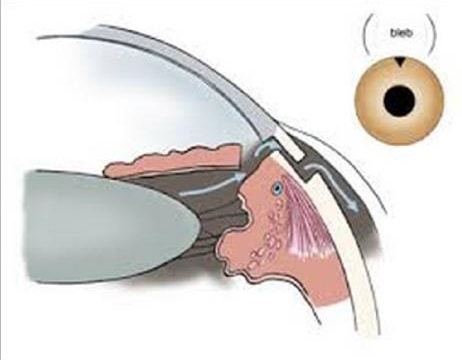
- Drainage implants: Some people with advanced, secondary, or childhood glaucoma may need drainage implants. In this procedure, a small tube is inserted to help drain fluid and lower eye pressure. Like trabeculectomy, the fluid forms a bleb—a small elevation on the white of the eye, often hidden under the eyelid.
Schedule a Consultation Today with Dr. Digvijay Singh for Glaucoma Treatment?
Should you have blurred vision, eye pressure, or the symptoms of glaucoma, you should seek consultation immediately. In Gurgaon, Dr. Digvijay Singh has been a trusted glaucoma specialist for many years, and our eye clinic is equipped with the latest instruments. Dr Singh dynamically crafts treatment plans for every single patient, offering glaucoma treatment in Gurgaon, and has a record with surgeries that are as non-intrusive as possible. Don’t wait until vision loss becomes irreversible; early detection and management are the key to controlling glaucoma eye disease. Book your appointment today with Dr. Singh, a trusted and best glaucoma specialist near me, and take the first step toward safeguarding your vision and long-term eye health.
FAQ About Glaucoma
Can glaucoma be cured permanently?
Glaucoma cannot be cured permanently, but early diagnosis and proper treatment can effectively control it. The aim of glaucoma treatment is to lower eye pressure and prevent further optic nerve damage. With regular checkups, medications, or surgery if needed, patients can maintain vision and avoid blindness caused by this progressive eye disease.
Who is at risk for developing glaucoma?
People over 40, those with a family history of glaucoma, individuals with high eye pressure, diabetics, and people of African or Asian descent are at higher risk. Other glaucoma risk factors include severe myopia, prolonged steroid use, and past eye injuries. Regular eye exams with a glaucoma specialist help detect the disease early.
Is glaucoma treatment painful or invasive?
Most glaucoma treatments are not painful or highly invasive. Eye drops are commonly prescribed to reduce eye pressure. If needed, laser procedures or minimally invasive surgeries are performed, usually with little discomfort. These treatments aim to preserve vision and are tailored to each patient’s condition and stage of glaucoma progression.
What are the early warning signs of glaucoma?
Glaucoma often develops silently without early symptoms, making it dangerous. Early signs may include blurred vision, eye pressure, halos around lights, or patchy blind spots. In acute cases, symptoms can be severe eye pain, headache, and nausea. Regular checkups with an eye doctor are crucial to detect glaucoma before vision loss occurs.
Will I lose my vision if I have glaucoma?
Glaucoma can cause permanent vision loss if left untreated. However, with early diagnosis and proper treatment, most patients maintain useful vision throughout life. Regular follow-ups with an ophthalmologist, adherence to medications, and timely procedures are key to preventing blindness. Effective glaucoma management ensures vision preservation for the long term.
How long does glaucoma treatment last?
Glaucoma treatment is usually lifelong because the condition is chronic and cannot be permanently cured. Medications, laser therapy, or surgeries aim to control eye pressure and slow progression. Patients need continuous monitoring, as stopping treatment can lead to vision damage. Ongoing care ensures stability and protection of eyesight over time.
I am suspected to have glaucoma. Now what?
If you are suspected to have glaucoma, regular follow-up is essential. Eye pressure should be checked 3–4 times a year. Fundus evaluation is done at every visit, visual field testing annually, and other tests like gonioscopy, corneal thickness measurement, and optic nerve imaging (HRT, GDx, OCT) may be needed.
How is eye pressure checked?
Tonometry measures the pressure inside the eye. Applanation tonometry is a contact method using anesthetic drops, a fluorescent dye, and a slit-lamp prism for accurate, painless measurement. Non-contact tonometry uses a puff of air on the eye to measure pressure without contact.
How often should you have an eye examination?
If you are diagnosed with glaucoma, it is important to visit your doctor at regular intervals (3 to 12 monthly follow up) to monitor your glaucoma. The duration of visits may be tailored by your treating eye doctor depending on the pressure control and the progression of visual field defects.
Does glaucoma lead to blindness?
If undiagnosed and untreated, glaucoma may lead to blindness. This is more so for angle closure type of glaucoma as compared to open angle type of glaucoma. But if diagnosed and properly treated, blindness can be prevented.
When is surgery done for glaucoma?
Surgery is done for glaucoma when the eye pressure is not getting controlled by medication or laser. It may be in the form of a trabeculectomy or a drainage implant.

